 |
 |
| Anim Biosci > Volume 36(3); 2023 > Article |
|
Abstract
Male fertility is affected by multiple endogenous stressors, including reactive oxygen species (ROS), which greatly deteriorate the fertility. However, physiological levels of ROS are required by sperm for the proper accomplishment of different cellular functions including proliferation, maturation, capacitation, acrosomal reaction, and fertilization. Excessive ROS production creates an imbalance between ROS production and neutralization resulting in oxidative stress (OS). OS causes male infertility by impairing sperm functions including reduced motility, deoxyribonucleic acid damage, morphological defects, and enhanced apoptosis. Several in-vivo and in-vitro studies have reported improvement in quality-related parameters of sperm following the use of different natural and synthetic antioxidants. In this review, we focus on the causes of OS, ROS production sources, mechanisms responsible for sperm damage, and the role of antioxidants in preserving sperm fertility.
Male fertility can be negatively impacted by multiple exogenous and endogenous stressors including reactive oxygen species (ROS). ROS are produced during oxygen metabolism either owning to the electron transport chain system or different conditions associated with enhanced energy demands. The highly reactive nature of ROS enables them to react with and modify any molecule through oxidation resulting in structural and functional alterations [1]. The most common type of produced ROS includes superoxide anion radicals (O2–•), hydrogen peroxide (H2O2), and hydroxyl radicals (OH•).
Recent reports have shown that ROS plays an important role in both reproductive physiology and pathology. This dual nature of ROS depends on the source, concentration, production site, and exposure time [2]. The physiological level of ROS is considered important for the proper accomplishment of different functions associated with gamete fertility including proliferation, maturation, the release of oocytes [3], capacitation, hyperactivation, acrosomal reaction, and fertilization [4]. However, ROS overproduction can trigger pathological responses damaging cells and tissues.
Living organisms are equipped with natural defense systems (antioxidants) to scavenge and neutralize the effects of ROS. Reports have verified the presence of a wide range of antioxidants in the seminal plasma that can protect sperm against the detrimental effects of ROS [5]. The enzymatic antioxidants present in the seminal plasma include superoxide dismutase (SOD), catalase (CAT), and glutathione peroxidase (GPx), whereas, non-enzymatic antioxidants include vitamins A and C, carnitine, glutathione (GSH), and pyruvate [5].
Under physiological conditions, an equilibrium is maintained in the male reproductive tract between ROS production and neutralization. However, excessive ROS production can overcome the antioxidant defense systems resulting in oxidative stress (OS). OS has been reported as a major cause of sperm damage affecting fertility [2]. The plasma membrane of the mammalian sperm is rich in polyunsaturated fatty acids (PUFAs) that increase vulnerability to oxidative damage [1]. Moreover, sperm with limited cell repair machinery lacks significant antioxidant protection owning to the limited volume and restricted cytoplasm distribution in the sperm cells [5].
Recent findings have shown that OS is associated with an increased percentage of damaged sperm due to the oxidation of deoxyribonucleic acid (DNA), lipids, proteins, and nucleotides [6]. Ultimately, the structural integrity of the plasma membrane is lost along with reduced sperm motility, an increase in morphological abnormalities, and cellular apoptosis [7]. Therefore, OS leads to infertility through impaired sperm function. The seminal plasma of fertile individuals shows greater antioxidant capacity than that of infertile ones [8]. One approach to control OS-induced damage is through the use of antioxidants that act by scavenging and neutralizing ROS. Over the years, researchers have used different antioxidants (natural and synthetic) either alone or combined and at different dosages for varying durations. Several in-vivo and in-vitro studies have reported beneficial outcomes achieved following antioxidant use including enhanced sperm concentration and motility, reduced morphological abnormalities and DNA fragmentation, better antioxidant capacity of seminal plasma, and improved outcomes of assisted reproductive biotechnologies [9]. However, in some cases, in-vitro improved sperm quality failed to improve fertility in clinical trials. In this review, we focus on the sources of ROS in semen, physiological and pathological effects of ROS on sperm, and the role of endogenous and exogenous antioxidants in preserving sperm fertility.
Sperm are the primary source of ROS produced in the semen. However, the amount of ROS produced depends on the maturation stage of sperm. In mature sperm, ROS production occurs either in the plasma membrane by nicotinamide adenine dinucleotide phosphate (NADPH) oxidase or in the presence of a nicotinamide adenine dinucleotide (NADH)-dependent oxidoreductase in the inner mitochondrial membrane, which ensures ROS production through electron leakage from the electron transport chain [10].
The leukocytes found in the semen are the second major source of ROS that acts as an integral part of the cellular defense system against infection, varicocele, spinal cord injury, and prolonged sexual absentia, and inflammation [10]. Leukocytic infiltration is enhanced during infection to counter infectious agents. Increased production of cytokines associated with inflammatory processes, such as interleukin-8, along with decreased production of SODs results in a respiratory burst and excessive ROS production leading to OS [11].
Excessive ROS production in the semen may be associated with certain extrinsic factors including the use of alcoholic drinks, air pollution, smoking, obesity, heat stress, toxicants or radiation exposure, aging, environmental factors, and nutritional deficiencies [12]. The ROS concentration in semen also depends on in-vitro techniques used for sperm washing. Pelleting sperm by cycles of centrifugation and resuspension induces ROS production [13].
For proper functioning and fertility, mammalian sperm need to acquire certain properties including normal morphology, motility, and capability to undergo different events such as capacitation and acrosomal reaction. Research evidence has shown that physiological levels of ROS act as intracellular signaling molecules necessary for different physiological processes including maturation, hyperactivation, capacitation, acrosomal reaction, and oocyte-sperm fusion [4]. A recent study reported that ROS levels in the semen of fertile individuals using chemiluminescence assay in terms of the mean±standard deviation and median 25th to 75th percentiles were 0.01±0.02×106 photons per minute (cpm)/20×106 sperm and 0.009 (0.004–0.014)×106 cpm/20×106 sperm [14]. During sperm maturation, a low magnitude of OS is required for other physiological events including mitochondrial activity, enhanced zona binding of sperm ROS are required for the proper packing of chromatin material essential for stability [15].
Sperm maturation occurs inside the ductus epididymis involving different steps such as alterations in the plasma membrane, rearrangement of membrane proteins, enzymatic modulations, and nuclear remodeling [16]. All of the above-mentioned steps are regulated through the appropriate signaling pathways modulated by the ROS present in the seminal plasma [17,18]. ROS are also involved in the formation of disulfide bonds to ensure chromatic stability and prevent damage to the chromosomal DNA.
Sperm capacitation and hyperactivation are considered prerequisite events to ensure successful fertilization. Reports have indicated two main changes occurring at the cellular level responsible for sperm capacitation including the generation of physiological levels of ROS and phosphorylation of protein tyrosine. It was found that ROS induces phosphorylation as in-vitro inhibition of ROS by the introduction of 2-deoxyglucose resulted in a reduced concentration of tyrosine-phosphorylated proteins [19]. The process is triggered by an influx of calcium (Ca2+) and bicarbonate ions. According to Du Plessis and his coworkers [17], both Ca2+ ions and ROS are involved in the initiation of the capacitation to cause the activation of adenylate cyclase which results in the production of cyclic adenosine monophosphate (cAMP). cAMP further causes the activation of downstream protein kinase A (PKA). PKA stimulates a membrane-bounded NADPH oxidase resulting in enhanced ROS production and phosphorylates serine and tyrosine, which leads to the activation of protein tyrosine kinase. ROS not only promotes the protein tyrosine kinase but also inhibits phosphotyrosine activity that normally dephosphorylates tyrosine. Protein tyrosine kinase phosphorylates tyrosine present in the fibrous sheath surrounding the axoneme of sperm flagellum. The enhanced phosphorylation of tyrosine is observed in the capacitation. A-kinase anchoring proteins are phosphorylated proteins that play a role in binding PKA with the fibrous sheath of the sperm [20] suggesting their possible involvement in the hyperactivity of sperm.
Following capacitation, the acrosome reaction is considered the last step of sperm maturation to acquire fertility [17]. The acrosome reaction is initiated by zona pellucida (ZP), progesterone hormone, and ROS. Acrosome reaction results in the release of acrosomal enzymes mainly acrosine from the sperm head that helps sperm in penetrating the ZP of the oocyte. Release of Ca2+ ions from the acrosome results in the breakdown of phosphatidylinositol-4-5-biphosphate yielding diacylglycerol (DAG) and inositol triphosphate. Inositol triphosphate causes the activation of actin-serving proteins that facilitates the fusion of the acrosome and plasma membrane of sperm to trigger exocytosis. Whereas, DAG triggers protein kinase C (PKC) activation leading to a greater influx of Ca2+ ions and activation of phospholipase A2 to release large amounts of fatty acids from the plasma membrane required for the fusion of sperm with the oocyte [21,22].
A proper level of H2O2 plays an important role in sperm function including sperm maturation, chromatin stability, capacitation, hyperactivation of sperm, and acrosome reaction, and increases the rate of sperm-oocyte fusion [23]. Furthermore, peroxides have been reported to be involved in the formation of a “mitochondrial capsule” that protects the mitochondria against proteolytic degradation [24]. Mitochondrial protection is essential for cellular metabolism, mediation of apoptosis, and ROS production. Recent reports have demonstrated that enhanced concentration of H2O2 is involved in sperm capacitation through the activation of adenylyl cyclase to produce cAMP which results in PKA-dependent phosphorylation of tyrosine residue [25]. According to Griveau and his co-workers, a 25 μM concentration of H2O2 enhanced sperm capacitation and hyperactivation following 3 h of incubation in B2 medium [26]. Contrary to the previous study, another study reported that a 50 μM concentration of H2O2 causes a twofold increase in cAMP production through adenylyl cyclase activation that leads to PKA-dependent protein tyrosine phosphorylation essential for capacitation [25].
O2–• is involved in sperm maturation, capacitation, acrosomal reaction, and sperm-oocyte fusion by enhancing the membrane fluidity of sperm [18]. Moreover, O2–• is the major species responsible for ROS-induced sperm hyperactivation possibly resulting from increased intracellular adenosine triphosphate (ATP) levels [27].
The role of O2–• in sperm capacitation was evident by the fact that O2–• produced during the incubation of sperm under capacitation conditions [28]. A study reported that during cryopreservation, O2–• improved the percentage of capacitated bovine sperms demonstrated by the induction of acrosome reaction using lysophosphatidylcholine [29]. Similar findings were reported by Zhang and Zheng [30] that exogenous O2–• significantly improved the percentage of human sperm that underwent capacitation (from 14.0±1.3 to 23.2±2.5) and acrosome reaction (from 4.5%±1.1% to 16%±2.0%, respectively). However, another study reported that no increase in the spontaneous acrosome reaction was observed following a direct addition of O2–• to the medium [21]. The presence of O2–• resulted in the production of unesterified fatty acids from the membranal phospholipids. Based on these findings it was suggested that O2–• secreted by sperm could be responsible for the ionophore-induced acrosome reaction via the de-esterification of membranel phospholipids [31].
Nitric oxide (NO•) is a free radical with a relatively long half-life. NO• production is catalyzed by nitric oxide synthase. NO• has been identified in the endothelium of testicular blood vessels. Physiological levels of NO• actively participate in signal transduction pathways responsible for sperm motility, capacitation, and acrosomal reaction and could stimulate the hyperactivation of mouse sperm [32].
NO• reported controlling sperm motility, at a low concentration of NO•, an increase in sperm motility has been observed. Whereas, moderate to high concentrations inversely affect sperm motility [33]. Hellstrom and his coworkers reported that a low level of sodium nitroprusside, a NO• producing compound improved sperm motility and viability due to reduced lipid peroxidation (LPO) [34]. Similar findings were observed in another study that low concentrations of sodium nitroprusside (10–7 and 10–8 M) significantly improved the percentage of capacitated sperm following 3 h of incubation [35]. Regulation of enzymatic activity might be the reason for the improved capacitation rate of sperm.
Furthermore, NO•-releasing compounds trigger the capacitation of human sperm but the effect on hyperactivation was not constant [36]. The effect of NO• on sperm capacitation was might be due to the oxidation of cellular components including membrane lipids or thiol groups either due to its direct reaction with H2O2 that leads to the formation of singlet oxygen or due to the oxidation of NO• to form nitrosonium cation that can react with H2O2 to yield peroxynitrite anion [37].
Research evidence has shown that NO• improves the binding of sperm with ZP. A study demonstrated that sperm treated with low concentrations of sodium nitroprusside (10–7 and 10–8 M) resulted in a significantly improved percentage of sperm binding with ZP following 3 h of incubation [35]. The effect of NO• on sperm-oocyte binding may be due to the interaction with H2O2 and O2–•.
Male infertility may be associated with excessive ROS production in semen. Excessive ROS production overcomes the antioxidant’s defense systems, disrupting the natural balance between ROS production and neutralization by antioxidants resulting in OS. In infertile individuals, ROS levels examined in the sperm samples in terms of the mean±standard deviation and median 25th to 75th percentiles were 0.35±0.67×106 cpm and 0.06 (0.02–0.33)×106 cpm/20×106 sperm [14]. OS produces pathological defects in major biomolecules including lipids, nucleic acids, proteins, and sugars [16]. The magnitude of oxidative damage depends on different factors including the nature and amount of ROS, duration of ROS exposure, temperature, oxygen tension, and composition of the surrounding environment (ions, proteins, and antioxidants) [38].
The plasma membrane of mammalian sperm is rich in PUFAs; fatty acids with more than two carbon-carbon double bonds [38]. These unconjugated double bonds are present between the methylene groups of PUFAs. The double bond near the methylene group reduces the strength of the methylene carbon-hydrogen bond, increasing hydrogen’s susceptibility to oxidative damage [39]. OS leads to a cascade of chemical reactions known as LPO. LPO is regarded as an autocatalytic self-propagating reaction that results in abnormal fertilization; it results in the loss of 60% of the fatty acids present in the plasma membrane, inversely affecting membrane fluidity, enhancing the permeability of ions, and inhibiting the actions of enzymes and receptors, as well as compromising sperm membrane integrity, defective motility, and reduced sperm-oocyte interaction [39].
OS causes severe damage to the nuclear material of sperm resulting in enhanced DNA fragmentation, modifications of base–pairs, chromatin cross-linking, and chromosomal microdeletions [11]. DNA damage results in cellular apoptosis, reduced fertilization rate, a higher percentage of miscarriage, and offspring mortality [40]. ROS-induced oxidative damage is also responsible for mutations in mitochondrial DNA that inversely affect sperm motility by inhibiting energy production. Agarwal et al [11] reported the involvement of at least one mitochondrial gene (of the 13) that codes for the electron transport chain system for reducing ATP and inducing intracellular ROS production. In infertile individuals, mature sperm are associated with higher ROS levels resulting in a significantly higher percentage of sperm undergoing apoptosis compared to the mature sperm of healthy individuals [41]. Reports have indicated a higher level of cytochrome C in the seminal fluids of infertile individuals, reflecting severe mitochondrial damage [6,11].
Antioxidants are compounds or enzymes that can dispose of, scavenge/neutralize, and inhibit ROS production or their actions. Antioxidants help to maintain cell function and structure by protecting the plasma membrane against ROS. Furthermore, antioxidant protects acrosome integrity preventing premature acrosome reaction. Antioxidants work by breaking the oxidative chain reaction resulting in reduced OS. Antioxidants can protect sperm from ROS produced by abnormal sperm or leukocytes, prevent DNA fragmentation and premature sperm maturation, reduce cryodamage, and improve sperm quality. We provide a summarized figure to illustrate the balance in ROS production on the physiological and pathological levels (Figure 1).
During spermatogenesis, sperm lose most of the cytoplasmic contents rendering a very low intracellular antioxidant capacity. Therefore, sperm protection against ROS mainly depends on the antioxidant capacity of the seminal plasma. Seminal plasma serves as the main barrier against extracellular ROS, containing different enzymatic and non-enzymatic antioxidant molecules including CAT, carotenoids (vitamin A), coenzyme Q 10 (CoQ10), GSH, GPx, GSH reductase, pyruvate, SOD, taurine, hypotaurine, uric acid, vitamin C, and vitamin E [5]. The antioxidant system of the body is affected by the dietary intake of antioxidants, minerals, and vitamins [42]. The use of antioxidants to neutralize the overproduction of ROS either directly into the semen extenders or inclusion in the diet has been well-researched and reported in the literature. In general, dietary antioxidants demand long-term and more persistent treatment protocols to benefit male fertility. The effect of each antioxidant depends on the dosage used and species of animal involved. Similarly, to preserve the integrity of sperm during freeze-thaw procedures, multiple relationships and mechanisms have been established. However, insights into how antioxidants serve protection and energy to sperm are still paradoxical. In this section, we focus on the role of endogenous antioxidants in preserving sperm fertility (Tables 1, 2).
SODs are metalloenzymes present in all life forms. SODs are considered an integral part of the antioxidant defense system that plays an active role in protecting sperm against OS. There are two main SOD isoforms including SOD-1 (75% of antioxidants) and SOD-3 (25% of antioxidants) that are derived from the prostate [43]. SOD protect cells against excessive O2–• levels by catalyzing the conversion of two O2–• into molecular oxygen and H2O2 [44]. Based on the presence of transition metal ions at the active site, SODs are classified into four main types: copper/zinc SOD, iron SOD, manganese SOD, and nickel SOD [45]. Peeker et al [43] reported that copper/zinc SOD is predominantly found in both sperm and seminal plasma.
In the male reproductive tract, SODs are secreted into the seminal plasma by the accessory sex glands, epididymis, sperm, and testicles (Sertoli and Leydig cells) and help maintain sperm motility for a long period [46]. Several reports have indicated that a SOD-supplemented semen extender could improve the freeze-thaw quality of bull [47] and stallion sperm [48]. In another study, supplementation of the canine freezing extender with SOD, CAT, and GPx preserved the quality of sperm obtained from fertile and sub-fertile dogs for 10 days at 4°C [49].
GPx is an important enzyme responsible for the detoxification of any lipid peroxide. GPx utilizes GSH as an electron donor to catalyze the reduction of H2O2 and O2–• [50]. GPx is regarded as superior to CAT in maintaining low cellular H2O2 [44]. The active site of GPx contains selenium in the form of selenocysteine [10]. GPx is found in both sperm and seminal plasma. In sperm, GPx is primarily located in the mitochondrial matrix whereas seminal GPx is suspected to originate from the prostate [51]. Moreover, GPx is expressed and secreted from the epididymal head into the semen [46]. The primary function of GPx is to protect the sperm plasma membrane against LPO, and sperm DNA from oxidative damage and chromatin condensation [50].
CAT is an enzyme found in the peroxisomes that decompose H2O2 into water and an oxygen molecule to prevent LPO of the plasma membrane. In semen, CAT was reported to be present in both sperm and seminal plasma. Seminal plasma is considered the main source of CAT; however, developing sperm also show a minimal level of CAT [52]. It was believed that CAT in the seminal plasma originated from the prostate gland [53]. The importance of CAT in seminal plasma is evident based on the observation that the semen of asthenozoospermic individuals may contain lower levels of CAT than that of normospermic individuals [46].
CAT supplementation reduced ROS levels and cryodamage in freeze-thaw sperm samples [54]. Moubasher et al [55] reported that supplementing fresh and processed semen with CAT results in improved freeze-thaw sperm motility, viability, and DNA integrity. Similarly, a CAT-supplemented semen extender prolonged sperm survival in camels [56]. Similar results were reported in another study when the freezing extender was supplemented with both CAT and SODs [57]. It was suspected that improvement in the freeze-thaw sperm quality was attributable to the combined and simultaneous action of both antioxidants against O2–• and H2O2 [57].
Carotenoids are fat-soluble organic compounds. Being precursors of vitamin A, carotenoids are mainly found in different vegetable dyes including orange, pink, red, and yellow. Carotenoids such as beta-carotenoids and lycopene are important components of the antioxidant defense system. Carotenoids help maintain the integrity of plasma membranes, regulate the proliferation of epithelial cells, and actively participate in spermatogenesis [58]. A carotenoid-deficient diet can lead to reduced sperm motility [10].
GSH is a natural antioxidant found in reproductive tract fluids and epididymal sperm semen of most of animal species and acts as a substrate in the peroxidase/reductase pathway to maintain the equilibrium and protect sperm from oxidative damage [59].
Reports have indicated that supplementation with GSH and its precursors (cysteine and glutamine) resulted in improved semen quality. In 1996, Irvine reported that the use of GSH for the treatment of infertile individuals with a varicocele or inflamed urogenital system resulted in significantly improved sperm quality [60]. In another study, a GSH-supplemented freezing extender improved the motility of donkey sperm by reducing the intracellular ROS levels [59]. However, GSH supplementation did not significantly affect other parameters of donkey sperm including plasma and acrosomal membrane integrity, mitochondrial membrane potential (MMP), and intracellular O2–• levels. Olfati Karaji and his co-workers reported improved freeze-thaw sperm quality by using a combination of GSH and SOD in the freezing extender of bull [61]. It was suspected that improved sperm quality was associated with reduced LPO and enhanced antioxidant levels.
Cysteine is a GSH precursor that can restore GSH depletion because of OS and inflammation [62]. In a clinical trial, oral intake of cysteine (600 mg/d) for 3 months improved the sperm quality and antioxidant status of infertile men [63]. Another report indicated that incubation of human sperm with cysteine for 2 h at room temperature significantly improved sperm motility [64]. Moreover, a cysteine-supplemented freezing extender protected sperm during the freeze-thaw procedure and resulted in improved sperm quality in bull [65], chicken [66], and ram [67] sperm.
Vitamin C is a naturally occurring water-soluble substance having outstanding antioxidant properties. Vitamin C protects sperm against oxidative damage by neutralizing O2–•, H2O2, and OH• [68]. Moreover, Vitamin C could effectively protect sperm DNA from ROS because of its high antioxidant competency [68]. The concentration of vitamin C is 10 times higher in seminal plasma than in the blood (364 vs 40 μmol/L) [10].
Several in-vivo studies have been performed to investigate the therapeutic potential of vitamin C for the restoration of fertility. Dawson et al [69] observed a positive correlation between vitamin C levels and sperm quality-related parameters including sperm concentration, motility, and viability. In that study, oral administration of vitamin C in smokers significantly improved the vitamin C levels in the seminal plasma and serum, resulting in improved semen quality. Similar findings were reported by Akmal et al [70] in infertile men with idiopathic oligozoospermia treated with vitamin C (2 gm/d). In another study, vitamin C supplementation (250 mg twice a day) resulted in improved sperm motility and morphology in patients following the surgical removal of varicocele [71]. However, vitamin C failed to improve the sperm count in such individuals. Vitamin C supplementation could effectively restore the fertility of rats with cyclophosphamide-induced testicular OS and androgenic disorders [72].
Furthermore, several in-vitro studies have reported improved sperm quality following the use of mediums supplemented with vitamin C. Inclusion of vitamin C (800 μmol/L) in the Ringer-Tyrode medium protected sperm from ROS-induced damage and improved sperm motility and viability [73]. However, higher concentrations of vitamin C (e.g. 1,000 μM) instead of protecting sperm against H2O2 increased the magnitude of oxidative damage. In another study, the supplementation of Percoll medium with vitamin C (600 μM) protected sperm DNA from damage [74]. Similar findings were obtained by another study where vitamin C-supplemented TEST yolk buffer failed to preserve sperm motility [31].
Vitamin E is a naturally occurring fat-soluble compound. Vitamin E is mainly present in the plasma membrane and possesses powerful chain-breaking antioxidant properties with dose-dependent effects. Vitamin E neutralizes free OH• and O2–• anions in the plasma membrane and reduces ROS-induced LPO. Therefore, vitamin E mainly protects the components of the sperm plasma membrane against LPO and improves the function of other antioxidants.
Different in-vivo studies have shown that vitamin E could be effectively used for the treatment of infertile individuals with oligoasthenozoospermia induced by OS [75,76]. Suleiman et al. observed that oral intake of vitamin E significantly increased the motile sperm count by decreasing malonic dialdehyde (end product of LPO) production from sperm [77]. In another study, Eid et al [78]. observed that vitamin E supplementation resulted in improved sperm concentration, motility, viability, and enhanced oxidative function in the seminal plasma of chickens [78].
Similarly, in-vitro studies have reported that vitamin E preserves sperm motility and also enhances their ability to penetrate hamster eggs [79]. During freeze-thaw procedures, the use of vitamin E-supplemented semen extenders at an inclusion rate of 10 mmol/L preserved sperm motility more efficiently compared to an untreated control group [31]. In 2003, Park and his coworkers reported that vitamin E supplementation resulted in reduced sperm damage and improved sperm motility during freeze-thaw procedures [80]. In another study, vitamin E-supplemented Percoll medium protected sperm DNA against oxidative damage [74].
Recent studies have shown that combined use of vitamins C and E together or alongwith other antioxidants can effectively improve semen quality. The oral intake of vitamins C and E can greatly reduce ROS-induced DNA damage in the sperm of normozoospermic and asthenozoospermic men [81]. Similarly, Greco et al. also observed reduced sperm DNA damage in infertile individuals following combined supplementation with vitamin C and vitamin E for 2 months [82]. It is believed that the use of hydrophilic vitamin C along with the lipophilic vitamin E results in a synergistic effect that reduces the magnitude of sperm damage induced by OS [83]. Similar findings were observed when vitamin C was used together with vitamin E and GSH [84]. Moreover, vitamin E combined with other antioxidants including β-carotene [85], vitamin C, GSH [86], and selenium [76,87] led to an improved semen profile in infertile individuals.
Taurine is a sulfur-containing amino acid that protects sperm against ROS when exposed to aerobic conditions or freeze-thaw procedures [88]. The antioxidant nature of taurine is related to its ability to elevate the CAT level in close association with the SOD concentration in bull, ram, and rabbit sperm [88].
An in-vivo study indicated that taurine use can significantly reverse the toxic effects of endosulfan in rats. Taurine treatment improved testicular weight, sperm count, motility, viability, and daily sperm production in endosulfan-treated rats [89].
An in-vitro study indicated that taurine and hypotaurine stimulate sperm capacitation and acrosomal reaction [90]. Furthermore, hypotaurine and taurine can inhibit spontaneous LPO in epididymal sperm [91]. Boatman et al [92] reported that hypotaurine restored the motility of hamster sperm affected by the washing procedure. Several studies have utilized taurine-supplemented semen extenders during different storage procedures. Storage of ram semen at room temperature using a taurine-supplemented extender significantly improved motility, membrane integrity, antioxidant status, and total antioxidant capacity [93]. Moreover, a taurine-supplemented semen extender showed the same protective effect during the chilling of tom [94], stallion [95], and donkey [96] sperm. Taurine supplementation resulted in improved freeze-thaw motility, viability, and plasma membrane integrity of buffalo [88], bull [97], and ram [98] sperm.
CoQ10 is a vitamin-like substance synthesized from tyrosine and serves as an important component of the inner mitochondrial membrane, an energy-promoting agent by supporting the mitochondrial electron transport chain, present in the mid-piece of the sperm tail. CoQ10 neutralizes O2–• and peroxides to protect lipids from oxidative damage. Gvozdjáková et al [99] reported that CoQ10 works by regenerating other antioxidants including vitamin E and vitamin C.
Several clinical trials have shown that CoQ10 supplementation resulted in improved semen quality in infertile individuals [100]. A meta-analysis of clinical trials investigating the effects of CoQ10 supplementation showed a significant improvement in sperm motility (total and progressive), sperm concentration, and seminal concentration of CoQ10 [101].
Some clinical trials have reported the beneficial effects of combined use of CoQ10 with other antioxidants. In male rats, oral intake of CoQ10 and L-carnitine attenuated the effects of high and oxidized low density lipoprotein (LDL) resulting in a significantly improved hormonal profile and sperm quality [102]. These improved outcomes may be attributable to efficient energy production from sperm mitochondria, which requires sufficient concentrations of CoQ10 and carnitine [99]. Gvozdjáková et al [99] reported that daily intake of CoQ10 (30 mg), L-carnitine (440 mg), vitamin C (12 mg), and vitamin E (75 IU) improved sperm concentration and pregnancy rates in infertile individuals.
In-vitro studies have shown the protective role of CoQ10 during freeze-thaw sperm procedures [103–105]. A CoQ10-supplemented freezing extender reduced the magnitude of cryodamage and resulted in the improved freeze-thaw quality of buck [106], fish [103], and ram [107] sperm. Similar results were observed when boar semen was stored at 17°C [108] and rooster semen was stored at 5°C [104] after being diluted with a CoQ10-supplemented semen extender. In contrast, a recent study showed that the addition of CoQ10 in the freezing extender of stallions did not affect the freeze-thaw sperm quality, but oral supplementation of stallions resulted in improved motility and membranal integrity of sperm after 24 h of cooling [109]. Similar findings were observed in another study where stallions were orally fed a diet supplemented with CoQ10 (1 gm/d) and improved semen quality was observed in the semen of five out of seven stallions following the cooling and freezing of semen [110].
Under normal conditions, endogenous antioxidant systems are primarily involved in the regulation of redox control. However, certain pathological conditions are associated with excessive ROS production overcoming redox control. In such circumstances, antioxidants from exogenous sources can play an important role in ameliorating the detrimental effects of OS. In this section, we focus on the role of exogenous antioxidants in preserving fertility (Table 3).
Astaxanthin (AXN) is a red keto-carotenoid pigment that has shown antioxidant activity against different oxidants and can inhibit LPO by penetrating biological membranes as well as suppresses ROS-induced damage to DNA, lipids, and proteins [111].
Several studies have reported that AXN has positive effects on fertility. An AXN-supplemented diet improved the osmolality, motility, concentration, and fertilization rate of sperm in goldfish [112]. In a clinical trial, Comhaire et al [113] reported that oral intake of AXN had a positive impact on semen quality and fertility of infertile individuals. In another study, oral intake of AXN combined with vitamins C and E ameliorated infertility in male rats [114]. AXN supplementation was reported to ameliorate the detrimental effects of diabetes on sperm parameters in rats [115].
Recent reports have confirmed the protective role of AXN during sperm preservation. AXN supplementation showed improved and protected sperm motility, viability, membrane integrity, and DNA during liquid preservation of boar [115] and ram [116] semen. Similar findings were observed during freeze-thaw procedures using an AXN-supplemented freezing extender in boar [117], dog [118], and ram [119] sperm.
Kinetin, a member of the cytokinin family has positive effects on cellular growth and division by reducing cycle length. Previous reports have indicated that kinetin can regulate the antioxidant activities of enzymes including CAT and SOD [120] resulting in reduced oxidative damage and is reported to reduce oxidative damage during in-vitro cell culture [121]. Recently, kinetin use was shown to be effective in alleviating cisplatin-induced testicular toxicity and organ damage by reducing OS, inflammation, and apoptosis [122]. During freeze-thaw procedures, the use of a kinetin-supplemented freezing extender resulted in improved sperm motility, viability, and structural integrity of dog [123] and ram [124] sperm.
Myo-inositol (MYO) is the most important naturally existing inositol and belongs to vitamin B complex group 1. MYO regulates the intracellular level of calcium ions and it has been suggested that MYO has a role in spermatogenesis and sperm function. Sertoli cells secrete MYO in response to the follicle-stimulating hormone that regulates different physiological events associated with sperm including maturation, motility, capacitation, and acrosomal reaction [125].
MYO has the potential to restore the fertility of male gametes and improve the fertilization rate [126]. In a clinical trial, oral intake of MYO resulted in improved sperm quality and balanced hormonal profiles in patients with idiopathic infertility [127]. Condorelli et al. suggested the use of MYO in infertile individuals based on the findings of their study that incubation of sperm in a medium supplemented with MYO (2 mg/mL) reduces the percentage of sperm with low MMP [128]. In another study, Condorelli et al. reported that MYO enhanced the motility of sperm retrieved following the swim-up procedure in both fertile and infertile individuals [129]. Furthermore, an MYO-supplemented freezing extender showed reduced OS and improved freeze-thaw sperm quality in different species including dogs [130], fish [131], bucks [132], and humans [133]. Similar results were observed when MYO supplementation was used during thawing procedures [134].
Quercetin (QR) is a flavonoid derived from plants and vegetables with strong antioxidant properties owing to the presence of three OH• groups. QR has been used to treat male infertility issues by scavenging ROS, as QR-supplemented sperm showed low levels of H2O2 [135]. Johinke et al [135] reported that sperm medium supplemented with QR protected against OS in 15°C-stored rabbit sperm over 96 h period. Moreover, recent studies have confirmed the protective role of QR against oxidative damage during the freeze-thaw procedure, as QR-supplemented freezing extender induced significant quality improvement in buck [136], bull [137], dog [138], human [139], and stallion [140] sperm.
Selenium is an essential component of a specific group of proteins known as selenoproteins. It is believed that the antioxidant nature of selenium is related to its ability to enhance GSH function. Selenium plays a major role in spermatogenesis and sperm maturation [141] and can protect sperm from ROS-induced DNA damage. The deficiency of selenium leads to certain defects such as mid-piece abnormalities and abnormal sperm motility [142]. Incubation of sperm from asthenoteratozoospermic individuals in a selenium-supplemented medium enhanced the percentage of motile sperm, sperm viability, and MMP [143]. Furthermore, selenium supplementation decreased LPO and DNA fragmentation.
Zinc (Zn2+) is an essential trace element that stimulates total antioxidant status, it helps reduce the production of H2O2 and OH• radicals through the neutralization of redox-active transition metals, such as iron and copper [144]. A recent study showed that Zn2+ can decrease DNA damage caused by the addition of H2O2 [145]. Fertile men have a significantly higher level of Zn2+ in the seminal plasma than subfertile men [146].
Zn2+ has a protective effect on sperm structure, as its deficiency leads to different tail defects including hypertrophy and hyperplasia of the fibrous sheath, axonemal disruption, defects of the inner microtubular dynein arms, and abnormal or absent mid-piece [147]. An in-vitro study reported that 10 μg/mL is the optimum concentration of Zn2+ that positively affects total and progressive sperm motility along with a reduction in DNA fragmentation and LPO [148]. Berkovitz et al [149] reported that Zn2+ supplementation before sperm freezing had beneficial effects on sperm motility and viability. They also observed improved sperm motility in freeze-thaw and in semen samples refrozen after thawing [149].
Sericin is a glue-like structure with strong antioxidant properties. Silkworm covers the silk filament with sericin to connect filaments and provide protection against a harmful environment. Recently, sericin has been used for liquid storage and freezing of sperm in different species including buck [150], bull [151], rabbit [152], and stallion [153]. Sericin supplementation resulted in an improved freeze-thaw sperm quality through an improved antioxidant status and reduced ROS level.
In the male reproductive system, ROS production is associated with different physiological and pathological conditions. ROS overproduction negatively influences fertility by disturbing the natural balance between ROS production and neutralization. OS-induced infertility appears to be a major challenge. Over the years, different antioxidant therapies have been utilized to address the infertility issues associated with OS either in the form of oral consumption or as in-vitro supplementation of different mediums. However, the outcomes of such studies appear to be controversial making it difficult to draw a conclusion. The reasons may include the low sample size used, differences in the concentrations used, and issues with the experimental designs. Moreover, the failure of antioxidants therapy can be attributed to the lack of real-time assessment methods and the inability to accurately quantify seminal OS.
To achieve better results, studies should be performed using larger sample sizes, classical pharmacological concentrations, and better-designed experiments. Furthermore, fertility can be recuperated using a combination of remedies (antioxidants, vitamins, trace minerals) along with knowledge of the underlying cause and severity of infertility. A new combination of antioxidants especially with polyphenols has shown a massive potential to treat infertility. Moreover, ROS levels in infertile individuals should always be correlated with the microenvironment of semen and reproduction outcomes (conception rate, quality of sperm functions, and embryo). This database will help in the development of reliable assays for the assessment of OS in reproductive cells and fluids.
Notes
CONFLICT OF INTEREST
We certify that there is no conflict of interest with any financial organization regarding the material discussed in the manuscript.
AUTHOR CONTRIBUTIONS
Conceptualization, AYQ, MIN, and JC; validation, AYQ, SR, and JC; formal analysis, PKR, and BMT; resources, AYQ, IMS, JC; writing—original draft preparation, AYQ, MIN, and SR; writing—review and editing, AYQ, IMS, and MIN; visualization, XF, PKR, SB, and BMT; supervision, JC; project administration, JC; funding acquisition, JC. All authors have read and agreed to the published version of the manuscript.
ACKNOWLEDGMENTS
We would like to acknowledge all members of our research team for their sincere contributions and the funding agency for their financial support.
Figure 1
The balance and impacts of reactive oxygen species (ROS) on sperm fertilizing ability. ROS can be released physiologically and on a minimal level they play a role in sperm maturation, capacitation, and acrosome reaction. Paradoxically, high levels of ROS damage the sperm membrane lipids and the nuclear DNA and lead to subfertility and infertility. The balance can be adjusted by administration of several kinds of antioxidants to treat the subfertility and infertility cases.
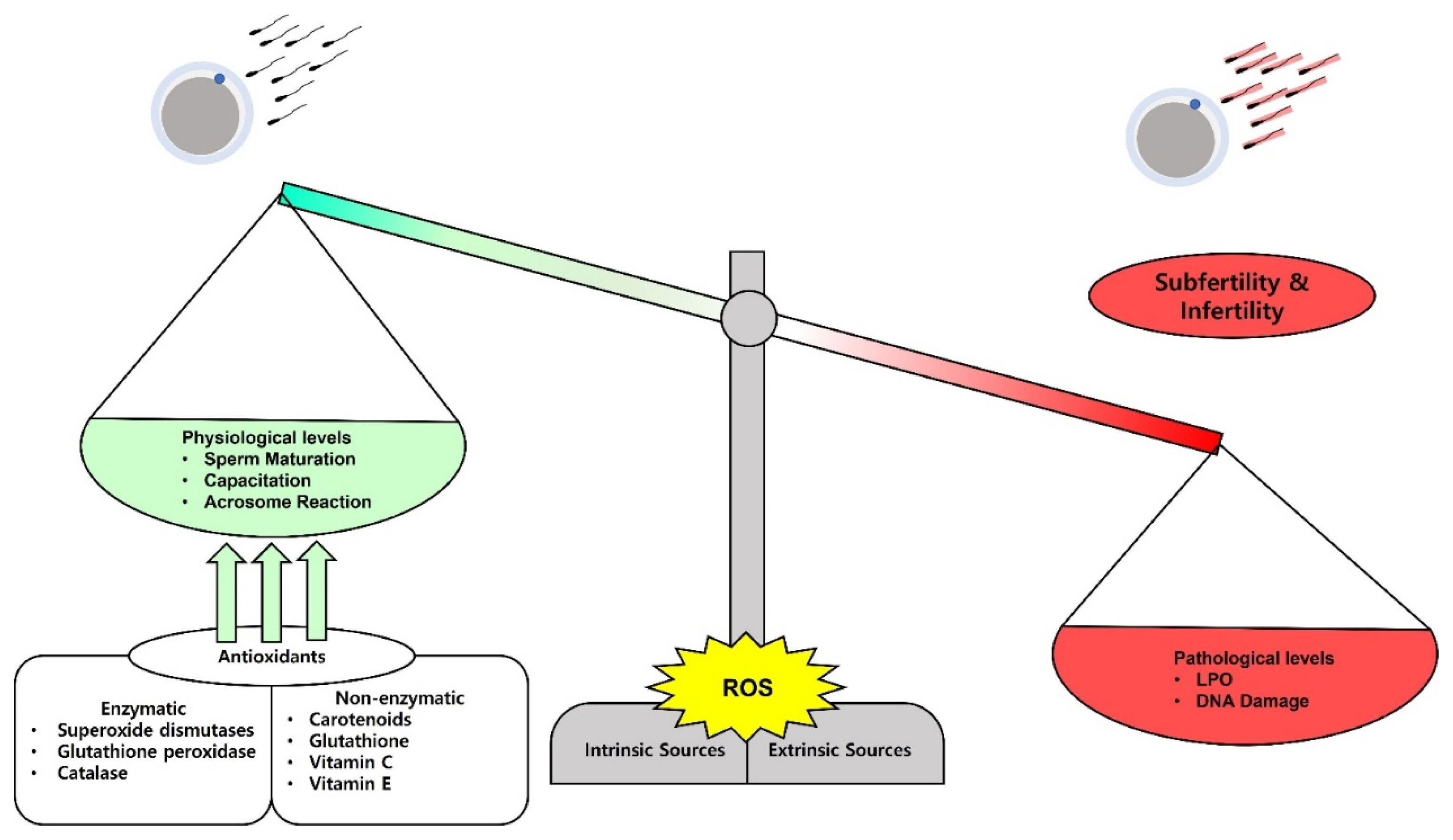
Table 1
Effects of endogenous-enzymatic antioxidants on male fertility
| Antioxidant | Study type | Specie | Dose used | Outcome | Reference |
|---|---|---|---|---|---|
| SOD | In-vitro | Stallion | 25, 50 U/mL | Improved progressive motility and viability of sperm | [48] |
| CAT | In-vitro | Human | 200 U/mL |
Higher progressive motile sperm Reduced DNA-damaged sperm |
[55] |
| Camel | 500 IU/mL | Higher total and progressive motile sperm | [56] | ||
| GPx, SOD | In-vitro | Bull |
0.0, 0.5, 1.0 mM 0, 250, 500 U/mL |
Non-return rates are 74% and 73.9% Improved sperm motility (6% to 11%) |
[154] |
| SOD, CAT, GPx | In-vitro | Dog | 15 IU/mL |
Higher progressive motile sperm Significantly higher DNA integrity |
[49] |
| Ascorbate & CAT | In-vitro | Human |
300, 600 μM 200, 400 U/mL |
Reduced significantly ROS levels in post-thaw sperm | [54] |
| SOD, CAT | In-vitro | Human | 200 U/mL |
Significantly improved sperm quality Reduced LPO |
[57] |
Table 2
Effect of endogenous non-enzymatic antioxidants on male fertility
| Antioxidant | Study type | Specie | Dose used | Outcome | Reference |
|---|---|---|---|---|---|
| GSH | In-vitro | Donkey | 0, 2, 4, 6, 8, 10 mM |
Significantly higher motility & kinematic parameters Higher sperm viability |
[59] |
| In-vivo | Human | 600 mg | Significantly improved fertility | [60] | |
| Reduced GSH & SOD | In-vitro | Bull |
GSH: 5, 7.5 mM SOD: 50, 100 U/mL |
Improved total and progressive motility parameters | [61] |
| Cysteine | In-vivo | Human | 600 mg |
Significantly improved sperm count and motility Significantly decreased abnormal morphology DNA fragmentation and protamine deficiency |
[63] |
| In-vitro | Human | 1.0 mg/mL |
Significantly improved sperm function and motility Significantly decreased ROS production |
[64] | |
| Buffalo | 0.0, 0.5, 1.0, 2.0, 3.0 mM | Improved antioxidant status, freeze-thaw quality, and in-vivo fertility | [65] | ||
| Cysteine & SOD | In-vitro | Chicken |
5 mM 200 U/mL |
Prevented the reduction in motility, viability, and mitochondrial membrane potential Protected sperm against apoptotic changes |
[66] |
| Cysteine & Erythioneine | In-vitro | Ram | 0, 1, 2, 4 mM | Improved freeze-thaw sperm motility and mitochondrial activity | [67] |
| Vitamin C | In-vivo | Human | 5, 10, 20, 60, 250 mg/d | Reduced oxidative DNA damage of sperm | [68] |
| 50, 100, 200, 400, 800, 1,000, 2,000, 4,000 μg | Improved sperm motility and viability through reduced ROS production | [73] | |||
| 0, 200, 1,000 mg/d | Improved sperm quality | [69] | |||
| 1,000 mg/d | Significant rise in sperm count, sperm motility, and sperm with normal morphology | [70] | |||
| 500 mg/d | Improved sperm motility and morphology | [71] | |||
| Rat | 25 mg/kg/d |
Protective role on cyclophosphamide-induced testicular dysfunction Alleviates the cyclophosphamide-induced OS |
[72] | ||
| 0.88 mg/kg | Higher sperm motility, viability, and count | [155] | |||
| Vitamin E | In-vivo | Chicken | 0, 20, 40, 80, 160 mg/kg |
Higher sperm viability and motility (40–160 mg/kg) Higher sperm concentration (80 mg/kg) |
[44] |
| 200 mg/kg diet |
Increased both sperm count and motility Reduced percentage of dead sperm |
[78] | |||
| Human | 600 mg/d | Significant improvement in in-vitro sperm function | [75] | ||
| 100 mg/d |
Significantly higher sperm motility Significantly decreased MDA levels |
[77] | |||
| Vitamins C & E | In-vivo | Human |
1,000 mg/d 800 mg/d |
Increased ejaculate volume, sperm count, and motility | [81] |
| 1,000 mg/d | Markedly reduced DNA-fragmented sperm | [82] | |||
| In-vitro | Human | 10 mM | Minimum improvement in sperm motility | [31] | |
| Vitamins C & E, CAT, Hypotaurine, Cysteine, GSH | In-vitro | Human |
0.2 and 1 mM 2,600 U/mL 1 & 10 mM 1 & 10 mM 1 & 10 mM |
Protects against OS | [83] |
| Vitamins C & E, GSH | In-vitro | Human | 200 mg, 200 mg, 400 mg | Reduced OS | [84] |
| Vitamins C & E, Urate, Cysteine | In-vitro | Human |
300, 600 μM 30, 60 μM 200, 400 μM 5, 10 μM |
Improved sperm DNA integrity | [74] |
| Mesterolone & Vitamin C | In-vivo | Human |
50 mg 200 mg |
No improvement in male fertility | [86] |
| Cysteine, Vitamin A, & Vitamin E | In-vivo | Human |
600 mg/d 30 and 180 mg/d |
Neutralized the ROS and improve sperm count No effect on sperm motility |
[85] |
| Selenium | In-vivo | Human | 100 μg/d | Significant rise in plasma selenium concentration and sperm motility | [156] |
|
400 U/d 200 μg/d |
Significantly higher sperm motility, viability, and fertility | [87] | |||
|
400 mg/d 225 μg/d |
Significantly improved sperm motility Significantly decreased MDA levels |
[76] | |||
| Rebamipide | In-vitro | Human | 10, 30, 100, 300 μM |
Decreased ROS level and LPO No effect on sperm viability |
[80] |
| Taurine | In-vitro | Sheep | 0, 10, 20, 40, 80, 100 mM | Reduced LPO and improved semen parameters | [93] |
| Cat | 50 mM | Higher sperm motility, Reduced abnormal sperms with sperm defects | [94] | ||
| Stallion | 70, 100 mM | Improved sperm survival | [95] | ||
| Donkey | 0, 20, 40, 60 mM | Significantly improved sperm motility | [96] | ||
| Hamster | 0, 2×10−3, 2×10−4, 2×10−5 M | Improved motility and promote capacitation | [90] | ||
| Hypotaurine | In-vitro | Hamster | 10 mM | Restore sperm motility and viability | [92] |
| Taurine & Hypotaurine | In-vitro | Rabbit | 0.5 mM | Reduced LPO and restored motility | [91] |
| Taurine & Trehalose | In-vitro | Cattle Bull |
50 mM 100 mM |
Significantly improved freeze-thaw motility, viability, and plasma membrane integrity | [97] |
| Buffalo Bull |
50 mM 100 mM |
Improved motility, viability, and membrane integrity Low numbers of capacitated sperm |
[88] | ||
| Taurine, QR, & GSH | In-vitro | Ram | 40 mM, 5 μg/mL, 5 mM |
Reduced LPO Improved freeze-thaw semen quality |
[98] |
| CoQ10 | In-vivo | Human | 200 mg/d |
Improved sperm concentration, progressive motility, total motility, and semen antioxidant status Reduced ROS level and SDF percentage |
[100] |
| Stallion | 1 gm/d | Improved semen quality | [110] | ||
| In-vivo & In-vitro | Human |
5, 50 μM 60 mg |
Improved sperm motility and fertilization rate | [157] | |
| Buffalo bull | 30 Mm | Improved sperm parameters and fertility | [105] | ||
| Rooster | 0, 1, 2, 5, 10 μM |
Significantly higher total sperm, progressive motilities, membrane functionality, viability, and mitochondria active potential Reduced LPO |
[104] | ||
| Buck | 0, 0.5, 1, 1.5 μM | Improved sperm motility, viability, and plasma membrane functionality | [106] | ||
| Giant grouper | 0, 25, 50, 100 μM | Improved total sperm motility, fertilization rate, and reduced DNA fragmentation | [103] | ||
| Boar | - | Increase the sperm characteristics and prolong the survival of liquid storage of sperm | [108] | ||
| Stallion | 40 & 80 μg/mL | No notable effect of semen quality | [109] | ||
| CoQ10 & L-carnitine | In-vivo | Rat |
10 mg/kg/d 350 mg/kg/d |
Significantly improved sperm quality and hormonal profile by weakening the high and oxidized LDL | [102] |
| CoQ10 & Ellagic acid | In-vitro | Ram |
0.5 μM 0.25 mM |
Higher total sperm, progressive motility, and viability No effect of sperm antioxidant level |
[107] |
Table 3
Use of exogenous antioxidants to improve the fertility of males
| Antioxidant | Route | Specie | Dose used | Outcome | Reference |
|---|---|---|---|---|---|
| AXN | In-vivo | Human | 0, 16 mg/kg | Positive effect on sperm parameters and fertility | [113] |
| 0.5, 1, 2 μM | Inhibited LPO | [158] | |||
| Ram | 0, 0.5, 1, 2, 4 μM |
Improved sperm vitality and membrane integrity Significantly reduced ROS production |
[116] | ||
| Rat | 720 mg/kg | Improved sperm viability, normal morphology, and DNA integrity | [115] | ||
| In-vitro | Boar | 0, 0.5, 1, 2, 5 μM | Improved freeze-thaw semen quality, inhibited LPO | [117] | |
| Dog | 0, 0.5, 1, 2 μM | Improved freeze-thaw sperm quality | [118] | ||
| Ram | 0, 0.5, 1, 2, 4 μM |
Decreased acrosome abnormalities Improve semen quality and fertility rate |
[119] | ||
| β-carotene & AXN | In-vivo | Goldfish | 50, 100, 150 mg/kg | Improved osmolality, motility, fertilization rate, and sperm concentration | [112] |
| AXN & Vitamins E and C | In-vivo | Rat |
100 mg/kg 100, and 200 mg/kg |
Improved fertility | [114] |
| Kinetin | In-vivo | Wheat Seedling | 1 μM | Improved growth, antioxidant, and chlorophyll content | [120] |
| Rat | 0.25, 0.5, 1 mg/kg |
Reduced organ damage and OS Inhibited the apoptosis |
[122] | ||
| In-vitro | Dog | 0, 25, 50, 100, 200 μM | Reduced OS and improved the freeze-thaw semen quality | [123] | |
| Ram | 0, 25, 50, 100, 200 μM | Enhanced sperm kinematics, viability, plasma membrane functionality, and reduced LPO | [124] | ||
| MYO | In-vivo & In-vitro | Human | 15 μL/mL | Improved sperm quality and motility | [126] |
| 2 g |
Increased acrosome-reacted sperm, sperm concentration, and progressive motility Optimized serum LH, FSH, and inhibin |
[127] | |||
|
No effect on mitochondrial function of sperm Increase sperm number with high MMP |
[128] | ||||
| Increase sperm motility and sperm number retrieved after swim-up | [129] | ||||
|
Improved total motility, progressive motility, and reduced DNA fragmentation Ineffective in inhibiting ROS level |
[133] | ||||
| 20 mg/mL |
Improvement of sperm vitality and motility Reduction of ROS-induced sperm defects |
[134] | |||
| Dog | 1, 2 mg/mL | Protected against OS and improved freeze-thaw sperm quality | [130] | ||
| Catfish | 5, 10, 20, 40 mg | Increased sperm motility, viability, and DNA integrity | [131] | ||
| MYO & Melatonin | In-vitro | Goat | - | Reduced ROS production, DNA damage, and LPO | [132] |
| In-vitro | Rabbit | 0, 25, 50, 100, 200 μM | Reduced H202 and LPO | [135] | |
| 50 μM | Higher sperm motility, viability, and DNA integrity | [139] | |||
| Goat | 10, 20 μM | Improves freeze-thaw sperm motion characteristics and inhibited LPO | [136] | ||
| Bull | 25, 50, 100, 200 μg/mL | No beneficial effect of motility, plasma membrane integrity, and sperm defects | [137] | ||
| Dog | 0, 25, 50, 100 μM | Reduced oxidative damage and improved the semen quality | [138] | ||
| 0.15 mM | Improved sperm motility and zona binding ability, reduced DNA fragmentation | [140] | |||
| Selenium | In vitro | Human | 2 μg/mL | Enhanced motility, viability, and MMP | [143] |
| Zn2+ | In-vitro | Human | 12.5 nM | Improved sperm parameters, and reduced DNA damage | [145] |
| 50 μM | Enhanced sperm total and progressive motility | [149] | |||
| Zn2+, D-aspartate, CoQ10 | In-vitro | Human |
1, 10, 100 μg/mL 5, 50, 500, 5,000 μg/mL 4, 40, 400 μg/mL |
Improved progressive sperm motility, reduced DNA fragmentation | [148] |
| Sericin | In-vitro | Buck | 0%, 0.25%, 0.5% | Ameliorated the freeze-thaw semen quality by improving the antioxidative status and minimizing the leakage of intracellular enzymes (0.25% Sericin) | [150] |
| Bull | 0%, 0.25%, 0.5%, 1.5%, 2% | Improved freeze-thaw semen quality by protecting against OS | [151] | ||
| Rabbit | 0%, 0.1%, 0.5% |
Enhanced osmotic tolerance and freeze-thaw sperm quality, Reduces the ability of rabbit sperm cells to undergo in-vitro-induced acrosome reaction, |
[152] | ||
| Stallion | 0.25% | Improved sperm DNA integrity and its resistance to ROS and LPO | [153] |
REFERENCES
1. Sanocka D, Kurpisz M. Reactive oxygen species and sperm cells. Reprod Biol Endocrinol 2004; 2:12
https://doi.org/10.1186/1477-7827-2-12



2. Aitken RJ, Smith TB, Jobling MS, Baker MA, De Iuliis GN. Oxidative stress and male reproductive health. Asian J Androl 2014; 16:31–8.
https://doi.org/10.4103/1008-682X.122203



3. Covarrubias L, Hernández-García D, Schnabel D, Salas-Vidal E, Castro-Obregón S. Function of reactive oxygen species during animal development: Passive or active? Dev Biol 2008; 320:1–11.
https://doi.org/10.1016/j.ydbio.2008.04.041


4. Baskaran S, Finelli R, Agarwal A, et al. Reactive oxygen species in male reproduction: A boon or a bane? Andrologia 2021; 53:e13577
https://doi.org/10.1111/and.13577


5. Saleh RA, Agarwal A. Oxidative stress and male infertility: From research bench to clinical practice. J Androl 2002; 23:737–52.
https://doi.org/10.1002/j.1939-4640.2002.tb02324.x


6. Aitken RJ, Gibb Z, Baker MA, et al. Causes and consequences of oxidative stress in spermatozoa. Reprod Fertil Dev 2016; 28:1–10.
https://doi.org/10.1071/RD15325


7. Schuppe HC, Meinhardt A, Allam J, Bergmann M, Weidner W, Haidl G. Chronic orchitis: A neglected cause of male infertility? Andrologia 2008; 40:84–91.
https://doi.org/10.1111/j.1439-0272.2008.00837.x


8. Subramanian V, Ravichandran A, Thiagarajan N, Govindarajan M, Dhandayuthapani S, Suresh S. Seminal reactive oxygen species and total antioxidant capacity: Correlations with sperm parameters and impact on male infertility. Clin Exp Reprod Med 2018; 45:88–93.
https://doi.org/10.5653/cerm.2018.45.2.88



9. Alahmar AT. The effects of oral antioxidants on the semen of men with idiopathic oligoasthenoteratozoospermia. Clin Exp Reprod Med 2018; 45:57–66.
https://doi.org/10.5653/cerm.2018.45.2.57



10. Walczak–Jedrzejowska R, Wolski JK, Slowikowska–Hilczer J. The role of oxidative stress and antioxidants in male fertility. Cent European J Urol 2013; 66:60–7.
https://doi.org/10.5173/ceju.2013.01.art19



11. Agarwal A, Virk G, Ong C, Plessis SS. Effect of oxidative stress on male reproduction. World J Mens Health 2014; 32:1–17.
https://doi.org/10.5534/wjmh.2014.32.1.1



12. Kang D, Kim D. Antioxidant effect of lonicera caerulea on heat stress-treated male mice. J Anim Reprod Biotechnol 2021; 36:220–9.
https://doi.org/10.12750/JARB.36.4.220

13. Alvarez JG, Lasso JL, Blasco L, et al. Centrifugation of human spermatozoa induces sublethal damage; separation of human spermatozoa from seminal plasma by a dextran swim-up procedure without centrifugation extends their motile lifetime. Hum Reprod 1993; 8:1087–92.
https://doi.org/10.1093/oxfordjournals.humrep.a138198


14. Desai N, Sharma R, Makker K, Sabanegh E, Agarwal A. Physiologic and pathologic levels of reactive oxygen species in neat semen of infertile men. Fertil Steril 2009; 92:1626–31.
https://doi.org/10.1016/j.fertnstert.2008.08.109


15. Sabeur K, Ball BA. Characterization of nadph oxidase 5 in equine testis and spermatozoa. Reproduction 2007; 134:263–70.
https://doi.org/10.1530/rep-06-0120


16. Thompson A, Agarwal A, Du Plessis SS. Physiological role of reactive oxygen species in sperm function: A review. Antioxidants in male infertility: a guide for clinicians and researchers. New York, USA: Springer Science and Business Media; 2013. p. 69–89.
17. Du Plessis SS, Agarwal A, Halabi J, Tvrda E. Contemporary evidence on the physiological role of reactive oxygen species in human sperm function. J Assist Reprod Genet 2015; 32:509–20.
https://doi.org/10.1007/s10815-014-0425-7



18. Griveau JF, Lannou DL. Reactive oxygen species and human spermatozoa: physiology and pathology. Int J Androl 1997; 20:61–9.
https://doi.org/10.1046/j.1365-2605.1997.00044.x


19. Aitken RJ, Harkiss D, Knox W, Paterson M, Irvine DS. A novel signal transduction cascade in capacitating human spermatozoa characterised by a redox-regulated, camp-mediated induction of tyrosine phosphorylation. J Cell Sci 1998; 111:645–56.
https://doi.org/10.1242/jcs.111.5.645


20. Leclerc P, de Lamirande E, Gagnon C. Cyclic adenosine 3′, 5monophosphate-dependent regulation of protein tyrosine phosphorylation in relation to human sperm capacitation and motility. Biol Reprod 1996; 55:684–92.
https://doi.org/10.1095/biolreprod55.3.684


21. Griveau JF, Renard P, Lannou DL. Superoxide anion production by human spermatozoa as a part of the ionophore-induced acrosome reaction process. Int J Androl 1995; 18:67–74.
https://doi.org/10.1111/j.1365-2605.1995.tb00388.x

22. Goldman R, Ferber E, Zort U. Reactive oxygen species are involved in the activation of cellular phospholipase A2. FEBS Lett 1992; 309:190–2.
https://doi.org/10.1016/0014-5793(92)81092-Z


23. Aitken RJ, Paterson M, Fisher H, Buckingham DW, van Duin M. Redox regulation of tyrosine phosphorylation in human spermatozoa and its role in the control of human sperm function. J Cell Sci 1995; 108:2017–25.
https://doi.org/10.1242/jcs.108.5.2017


24. Roveri A, Ursini F, Flohé L, Maiorino M. PHGPx and spermatogenesis. Biofactors 2001; 14:213–22.
https://doi.org/10.1002/biof.5520140127


25. Rivlin J, Mendel J, Rubinstein S, Etkovitz N, Breitbart H. Role of hydrogen peroxide in sperm capacitation and acrosome reaction. Biol Reprod 2004; 70:518–22.
https://doi.org/10.1095/biolreprod.103.020487


26. Griveau J, Renard P, Lannou DL. An in vitro promoting role for hydrogen peroxide in human sperm capacitation. Int J Androl 1994; 17:300–7.
https://doi.org/10.1111/j.1365-2605.1994.tb01260.x


27. Williams AC, Ford WC. The role of glucose in supporting motility and capacitation in human spermatozoa. J Androl 2001; 22:680–95.
https://doi.org/10.1002/j.1939-4640.2001.tb02229.x


28. de Lamirande E, Gagnon C. Capacitation-associated production of superoxide anion by human spermatozoa. Free Radic Biol Med 1995; 18:487–95.
https://doi.org/10.1016/0891-5849(94)00169-K


29. O’Flaherty C, Beorlegui N, Beconi MT. Participation of superoxide anion in the capacitation of cryopreserved bovine sperm. Int J Androl 2003; 26:109–14.
https://doi.org/10.1046/j.1365-2605.2003.00404.x


30. Zhang H, Zheng RL. Promotion of human sperm capacitation by superoxide anion. Free Radic Res 2009; 24:261–8.
https://doi.org/10.3109/10715769609088023

31. Askari H, Check J, Peymer N, Bollendorf A. Effect of natural antioxidants tocopherol and ascorbic acids in maintenance of sperm activity during freeze-thaw process. Arch Androl 1994; 33:11–5.
https://doi.org/10.3109/01485019408987797


32. Herrero MB, Cebral E, Boquet M, Viggiano JM, Vitullo A, Gimeno MA. Effect of nitric oxide on mouse sperm hyperactivation. Acta Physiol Pharmacol Ther Latinoam 1994; 44:65–9.

33. Francavilla F, Santucci R, Macerola B, Ruvolo G, Romano R. Nitric oxide synthase inhibition in human sperm affects sperm-oocyte fusion but not zona pellucida binding. Biol Reprod 2000; 63:425–9.
https://doi.org/10.1095/biolreprod63.2.425


34. Hellstrom WJ, Bell M, Wang R, et al. Effect of sodium nitroprusside on sperm motility, viability, and lipid peroxidation. Fertil Steril 1994; 61:1117–22.
https://doi.org/10.1016/S0015-0282(16)56766-1


35. Sengoku K, Tamate K, Yoshida T, Takaoka Y, Miyamoto T, Ishikawa M. Effects of low concentrations of nitric oxide on the zona pellucida binding ability of human spermatozoa. Fertil Steril 1998; 69:522–7.
https://doi.org/10.1016/S0015-0282(97)00537-2


36. Zini A, de Lamirande E, Gagnon C. Low levels of nitric oxide promote human sperm capacitation in vitro. J Androl 1995; 16:424–31.
https://doi.org/10.1002/j.1939-4640.1995.tb00558.x


37. Stamler JS, Singel DJ, Loscalzo J. Biochemistry of nitric oxide and its redox-activated forms. Science 1992; 258:1898–902.
https://doi.org/10.1126/science.1281928


38. Agarwal A, Makker K, Sharma R. Clinical relevance of oxidative stress in male factor infertility: an update. Am J Reprod Immunol 2008; 59:2–11.
https://doi.org/10.1111/j.1600-0897.2007.00559.x


39. Dutta S, Majzoub A, Agarwal A. Oxidative stress and sperm function: A systematic review on evaluation and management. Arab J Urol 2019; 17:87–97.
https://doi.org/10.1080/2090598X.2019.1599624



40. Chen SJ, Allam JP, Duan YG, Haidl G. Influence of reactive oxygen species on human sperm functions and fertilizing capacity including therapeutical approaches. Arch Gynecol Obstet 2013; 288:191–9.
https://doi.org/10.1007/s00404-013-2801-4


41. Agarwal A, Said TM. Role of sperm chromatin abnormalities and DNA damage in male infertility. Hum Reprod Update 2003; 9:331–45.
https://doi.org/10.1093/humupd/dmg027


42. Agarwal A, Gupta S, Sharma RK. Role of oxidative stress in female reproduction. Reprod Biol Endocrinol 2005; 3:28
https://doi.org/10.1186/1477-7827-3-28



43. Peeker R, Abramsson L, Marklund SL. Superoxide dismutase isoenzymes in human seminal plasma and spermatozoa. Mol Hum Reprod 1997; 3:1061–6.
https://doi.org/10.1093/molehr/3.12.1061


44. Lin YF, Chang SJ, Yang JR, Lee YP, Hsu AL. Effects of supplemental vitamin e during the mature period on the reproduction performance of taiwan native chicken cockerels. Br Poult Sci 2005; 46:366–73.
https://doi.org/10.1080/00071660500098186


45. Youn HD, Kim EJ, Roe JH, Hah YC, Kang SO. A novel nickel-containing superoxide dismutase from streptomyces spp. Biochem J 1996; 318:889–96.
https://doi.org/10.1042/bj3180889



46. Chen H, Chow PH, Cheng SK, Cheung ALM, Cheng LYL, O WS. Male genital tract antioxidant enzymes: Their source, function in the female, and ability to preserve sperm DNA integrity in the golden hamster. J Androl 2003; 24:704–11.
https://doi.org/10.1002/j.1939-4640.2003.tb02730.x


47. Asadpour R, Jafari R, Tayefi NH. The effect of antioxidant supplementation in semen extenders on semen quality and lipid peroxidation of chilled bull spermatozoa (short paper). Iranian J Vet Res 2012; 13:246–9.
48. Cocchia N, Pasolini MP, Mancini R, et al. Effect of sod (superoxide dismutase) protein supplementation in semen extenders on motility, viability, acrosome status and erk (extracellular signal-regulated kinase) protein phosphorylation of chilled stallion spermatozoa. Theriogenology 2011; 75:1201–10.
https://doi.org/10.1016/j.theriogenology.2010.11.031


49. Del Prete C, Ciani F, Tafuri S, et al. Effect of superoxide dismutase, catalase, and glutathione peroxidase supplementation in the extender on chilled semen of fertile and hypofertile dogs. J Vet Sci 2018; 19:667–75.
https://doi.org/10.4142/jvs.2018.19.5.667



50. Tavilani H, Goodarzi MT, Doosti M, et al. Relationship between seminal antioxidant enzymes and the phospholipid and fatty acid composition of spermatozoa. Reprod Biomed Online 2008; 16:649–56.
https://doi.org/10.1016/S1472-6483(10)60478-6


51. Yeung CH, Cooper TG, De Geyter M, et al. Studies on the origin of redox enzymes in seminal plasma and their relationship with results of in-vitro fertilization. Mol Hum Reprod 1998; 4:835–9.
https://doi.org/10.1093/molehr/4.9.835


52. Bauché F, Fouchard MH, Jégou B. Antioxidant system in rat testicular cells. FEBS Lett 1994; 349:392–6.
https://doi.org/10.1016/0014-5793(94)00709-8


53. Fraczek M, Kurpisz M. The redox system in human semen and peroxidative damage of spermatozoa. Postepy Hig Med Dosw 2005; 59:523–34.
54. Li Z, Lin Q, Liu R, Xiao W, Liu W. Protective effects of ascorbate and catalase on human spermatozoa during cryopreservation. J Androl 2010; 31:437–44.
https://doi.org/10.2164/jandrol.109.007849


55. Moubasher AE, El Din AME, Ali ME, El-sherif WT, Gaber HD. Catalase improves motility, vitality and DNA integrity of cryopreserved human spermatozoa. Andrologia 2013; 45:135–9.
https://doi.org/10.1111/j.1439-0272.2012.01310.x


56. Malo C, Grundin J, Morrell JM, Skidmore JA. Individual male dependent improvement in post-thaw dromedary camel sperm quality after addition of catalase. Anim Reprod Sci 2019; 209:106168
https://doi.org/10.1016/j.anireprosci.2019.106168


57. Rossi T, Mazzilli F, Delfino M, Dondero F. Improved human sperm recovery using superoxide dismutase and catalase supplementation in semen cryopreservation procedure. Cell Tissue Ban 2001; 2:9–13.
https://doi.org/10.1023/A:1011592621487

58. Hogarth CA, Griswold MD. The key role of vitamin a in spermatogenesis. J Clin Invest 2010; 120:956–62.
https://doi.org/10.1172/JCI41303



59. Yánez-Ortiz I, Catalán J, Delgado-Bermúdez A, Carluccio A, Miró J, Yeste M. Addition of reduced glutathione (gsh) to freezing medium reduces intracellular ros levels in donkey sperm. Vet Sci 2021; 8:302
https://doi.org/10.3390/vetsci8120302



60. Irvine DS. Glutathione as a treatment for male infertility. Rev Reprod 1996; 1:6–12.
https://doi.org/10.1530/revreprod/1.1.6


61. Olfati Karaji R, Daghigh Kia H, Ashrafi I. Effects of in combination antioxidant supplementation on microscopic and oxidative parameters of freeze–thaw bull sperm. Cell Tissue Ban 2014; 15:461–70.
https://doi.org/10.1007/s10561-013-9412-y

62. Wang F, Liu S, Shen Y, et al. Protective effects of n‐acetylcysteine on cisplatin‐induced oxidative stress and DNA damage in hepg2 cells. Exp Ther Med 2014; 8:1939–45.
https://doi.org/10.3892/etm.2014.2019



63. Jannatifar R, Parivar K, Roodbari NH, Nasr-Esfahani MH. Effects of n-acetyl-cysteine supplementation on sperm quality, chromatin integrity and level of oxidative stress in infertile men. Reprod Biol Endocrinol 2019; 17:24
https://doi.org/10.1186/s12958-019-0468-9



64. Oeda T, Henkel R, Ohmori H, Schill WB. Scavenging effect of n-acetyl-l-cysteine against reactive oxygen species in human semen: A possible therapeutic modality for male factor infertility? Andrologia 1997; 29:125–31.
https://doi.org/10.1111/j.1439-0272.1997.tb00305.x


65. Beheshti R, Asadi A, Eshratkhah B, et al. The effect of cysteine on post-thawed buffalo bull (bubalus bubalis) sperm parameters. Adv Environ Biol 2011; 5:1260–3.
66. Partyka A, Niżański W, Bajzert J, Łukaszewicz E, Ochota M. The effect of cysteine and superoxide dismutase on the quality of post-thawed chicken sperm. Cryobiology 2013; 67:132–6.
https://doi.org/10.1016/j.cryobiol.2013.06.002


67. Çoyan K, Başpınar N, Bucak MN, Akalın PP. Effects of cysteine and ergothioneine on post-thawed merino ram sperm and biochemical parameters. Cryobiology 2011; 63:1–6.
https://doi.org/10.1016/j.cryobiol.2011.04.001


68. Fraga CG, Motchnik PA, Shigenaga MK, Ames BN. Ascorbic acid protects against endogenous oxidative DNA damage in human sperm. Proc Natl Acad Sci 1991; 88:11003–6.
https://doi.org/10.1073/pnas.88.24.11003



69. Dawson EB, Harris WA, Teter MC, Powell LC. Effect of ascorbic acid supplementation on the sperm quality of smokers. Fertil Steril 1992; 58:1034–9.
https://doi.org/10.1016/S0015-0282(16)55456-9


70. Akmal M, Qadri JQ, Al-Waili NS, Thangal S, Haq A, Saloom KY. Improvement in human semen quality after oral supplementation of vitamin C. J Med Food 2006; 9:440–2.
https://doi.org/10.1089/jmf.2006.9.440


71. Cyrus A, Kabir A, Goodarzi D, Moghimi M. The effect of adjuvant vitamin c after varicocele surgery on sperm quality and quantity in infertile men: A double blind placebo controlled clinical trial. Int Braz J Urol 2015; 41:230–8.
https://doi.org/10.1590/S1677-5538.IBJU.2015.02.07



72. Das UB, Mallick M, Debnath JM, Ghosh D. Protective effect of ascorbic acid on cyclophosphamide-induced testicular gametogenic and androgenic disorders in male rats. Asian J Androl 2002; 4:201–8.

73. Verma A, Kanwar KC. Human sperm motility and lipid peroxidation in different ascorbic acid concentrations: An in vitro analysis. Andrologia 1998; 30:325–9.
https://doi.org/10.1111/j.1439-0272.1998.tb01178.x


74. Hughes CM, Lewis SE, McKelvey-Martin VJ, Thompson W. The effects of antioxidant supplementation during percoll preparation on human sperm DNA integrity. Hum Reprod 1998; 13:1240–7.
https://doi.org/10.1093/humrep/13.5.1240


75. Kessopoulou E, Powers HJ, Sharma KK, et al. A double-blind randomized placebo cross-over controlled trial using the antioxidant vitamin e to treat reactive oxygen species associated male infertility. Fertil Steril 1995; 64:825–31.
https://doi.org/10.1016/S0015-0282(16)57861-3


76. Keskes-Ammar L, Feki-Chakroun N, Rebai T, et al. Sperm oxidative stress and the effect of an oral vitamin e and selenium supplement on semen quality in infertile men. Arch Androl 2003; 49:83–94.
https://doi.org/10.1080/01485010390129269


77. Suleiman SA, Ali ME, Zaki Z, El-Malik EMA, Nasr MA. Lipid peroxidation and human sperm motility: Protective role of vitamin E. J Androl 1996; 17:530–7.
https://doi.org/10.1002/j.1939-4640.1996.tb01830.x


78. Eid Y, Ebeid T, Younis H. Vitamin e supplementation reduces dexamethasone-induced oxidative stress in chicken semen. Br Poult Sci 2006; 47:350–6.
https://doi.org/10.1080/00071660600753912


79. De Lamirande E, Gagnon C. Reactive oxygen species and human spermatozoa. I. Effects on the motility of intact spermatozoa and on sperm axonemes. J Androl 1992; 13:368–78.
https://doi.org/10.1002/j.1939-4640.1992.tb03327.x


80. Park NC, Park HJ, Lee KM, Shin DG. Free radical scavenger effect of rebamipide in sperm processing and cryopreservation. Asian J Androl 2003; 5:195–202.

81. Rolf C, Cooper T, Yeung C, Nieschlag E. Antioxidant treatment of patients with asthenozoospermia or moderate oligoasthenozoospermia with high-dose vitamin c and vitamin e: a randomized, placebo-controlled, double-blind study. Hum Reprod 1999; 14:1028–33.
https://doi.org/10.1093/humrep/14.4.1028


82. Greco E, Iacobelli M, Rienzi L, Ubaldi F, Ferrero S, Tesarik J. Reduction of the incidence of sperm DNA fragmentation by oral antioxidant treatment. J Androl 2005; 26:349–53.
https://doi.org/10.2164/jandrol.04146


83. Baker HG, Brindle J, Irvine DS, Aitken RJ. Protective effect of antioxidants on the impairment of sperm motility by activated polymorphonuclear leukocytes. Fertil Steril 1996; 65:411–9.
https://doi.org/10.1016/S0015-0282(16)58109-6


84. Kodama H, Yamaguchi R, Fukuda J, Kasai H, Tanaka T. Increased oxidative deoxyribonucleic acid damage in the spermatozoa of infertile male patients. Fertil Steril 1997; 68:519–24.
https://doi.org/10.1016/S0015-0282(97)00236-7


85. Comhaire FH, Christophe AB, Zalata AA, Dhooge WS, Mahmoud AMA, Depuydt CE. The effects of combined conventional treatment, oral antioxidants and essential fatty acids on sperm biology in subfertile men. Prostaglandins Leukot Essent Fatty Acids 2000; 63:159–65.
https://doi.org/10.1054/plef.2000.0174


86. Hargreave T, Kyle K, Baxby K, et al. Randomised trial of mesterolone versus vitamin c for male infertility. Br J Urol 1984; 56:740–4.
https://doi.org/10.1111/j.1464-410X.1984.tb06160.x


87. Moslemi MK, Tavanbakhsh S. Selenium–vitamin e supplementation in infertile men: effects on semen parameters and pregnancy rate. Int J Gen Med 2011; 4:99–104.
https://doi.org/10.2147/IJGM.S16275



88. Reddy NSS, Mohanarao GJ, Atreja SK. Effects of adding taurine and trehalose to a tris-based egg yolk extender on buffalo (bubalus bubalis) sperm quality following cryopreservation. Anim Reprod Sci 2010; 119:183–90.
https://doi.org/10.1016/j.anireprosci.2010.01.012


89. Aly HAA, Khafagy RM. Taurine reverses endosulfan-induced oxidative stress and apoptosis in adult rat testis. Food Chem Toxicol 2014; 64:1–9.
https://doi.org/10.1016/j.fct.2013.11.007


90. Mrsny RJ, Waxman L, Meizel S. Taurine maintains and stimulates motility of hamster sperm during capacitation in vitro. J Exp Zool 1979; 210:123–8.
https://doi.org/10.1002/jez.1402100113


91. Alvarez JG, Storey BT. Taurine, hypotaurine, epinephrine and albumin inhibit lipid peroxidation in rabbit spermatozoa and protect against loss of motility. Biol Reprod 1983; 29:548–55.
https://doi.org/10.1095/biolreprod29.3.548


92. Boatman DE, Bavister BD, Cruz E. Addition of hypotaurine can reactivate immotile golden hamster spermatozoa. J Androl 1990; 11:66–72.
https://doi.org/10.1002/j.1939-4640.1990.tb01581.x


93. Zhang L, Wang Y, Sohail T, et al. Effects of taurine on sperm quality during room temperature storage in hu sheep. Animals 2021; 11:2725
https://doi.org/10.3390/ani11092725



94. Baran A, Demir K, Şahin BE, et al. Short-term chilled storage of cat semen extended with and without taurine containing milk extenders. J Anim Vet Adv 2009; 8:1367–71.
95. Ijaz A, Ducharme R. Effect of various extenders and taurine on survival of stallion sperm cooled to 5°C. Theriogenology 1995; 44:1039–50.
https://doi.org/10.1016/0093-691X(95)00290-O


96. Dorado J, Acha D, Ortiz I, et al. Effect of extender and amino acid supplementation on sperm quality of cooled-preserved andalusian donkey (equus asinus) spermatozoa. Anim Reprod Sci 2014; 146:79–88.
https://doi.org/10.1016/j.anireprosci.2014.02.009


97. Chhillar S, Singh VK, Kumar R, Atreja SK. Effects of taurine or trehalose supplementation on functional competence of cryopreserved karan fries semen. Anim Reprod Sci 2012; 135:1–7.
https://doi.org/10.1016/j.anireprosci.2012.08.029


98. Banday MN, Lone FA, Rasool F, Rashid M, Shikari A. Use of antioxidants reduce lipid peroxidation and improve quality of crossbred ram sperm during its cryopreservation. Cryobiology 2017; 74:25–30.
https://doi.org/10.1016/j.cryobiol.2016.12.008


99. Gvozdjáková A, Kucharská J, Dubravicky J, Mojto V, Singh RB. Coenzyme q10, α-tocopherol, and oxidative stress could be important metabolic biomarkers of male infertility. Dis Markers 2015; 2015:827941
https://doi.org/10.1155/2015/827941



100. Alahmar AT, Calogero AE, Sengupta P, Dutta S. Coenzyme q10 improves sperm parameters, oxidative stress markers and sperm DNA fragmentation in infertile patients with idiopathic oligoasthenozoospermia. World J Mens Health 2021; 39:346–51.
https://doi.org/10.5534/wjmh.190145



101. Lafuente R, González-Comadrán M, Solà I, et al. Coenzyme q10 and male infertility: a meta-analysis. J Assist Reprod Genet 2013; 30:1147–56.
https://doi.org/10.1007/s10815-013-0047-5



102. Ghanbarzadeh S, Garjani A, Ziaee M, Khorrami A. Coq10 and l-carnitine attenuate the effect of high ldl and oxidized ldl on spermatogenesis in male rats. Drug Res 2014; 64:510–5.
https://doi.org/10.1055/s-0033-1361176

103. Yang S, Fan B, Chen X, Meng Z. Supplementation of the freezing medium with coenzyme q10 attenuates oxidative stress and improves function of frozen-thawed giant grouper (epinephelus lanceolatus) spermatozoa. Theriogenology 2021; 175:77–82.
https://doi.org/10.1016/j.theriogenology.2021.08.029


104. Masoudi R, Sharafi M, Pourazadi L. Improvement of rooster semen quality using coenzyme q10 during cooling storage in the lake extender. Cryobiology 2019; 88:87–91.
https://doi.org/10.1016/j.cryobiol.2019.03.003


105. Doidar Y, El-Nagar H, Elrefy A, Mousbah AM. Cryopreservation and quality assessment of buffalo bull (bubalus bubalis) semen using new moringa extender and antioxidant co-q10. J Anim Poult Prod 2018; 9:375–81.

106. Yousefian I, Emamverdi M, Karamzadeh-Dehaghani A, Sabzian-Melei R, Zhandi M, Zare-Shahneh A. Attenuation of cryopreservation-induced oxidative stress by antioxidant: Impact of coenzyme q10 on the quality of post-thawed buck spermatozoa. Cryobiology 2018; 81:88–93.
https://doi.org/10.1016/j.cryobiol.2018.02.005


107. Daghigh Kia H, Bolooki Z, Vaseghi Dodran H, et al. Effect of adding coenzyme q10 and ellagic acid during cryopreservation on post-thaw quality of ram semen. Iran J Appl Anim Sci 2017; 7:445–51.
108. Pîndaru LP, Cenariu M, Pall E, et al. Effects of coenzyme q10 on sperm viability during storage of boar semen at 17°C. Sci Works Ser C Vet Med 2015; 61:32–6.
109. Olivieri AJR. Effects of coenzyme q10 (coq10) supplementation on equine semen quality. Pullman, WA, USA: Washington State University; 2019.
110. Ruiz AJ, Tibary A, Heaton RA, Hargreaves IP, Leadon DP, Bayly WM. Effects of feeding coenzyme q10-ubiquinol on plasma coenzyme q10 cocentrations and semen quality in sallions. J Equine Vet Sci 2021; 96:103303
https://doi.org/10.1016/j.jevs.2020.103303


111. Palozza P, Krinsky NI. Astaxanthin and canthaxanthin are potent antioxidants in a membrane model. Arch Biochem Biophys 1992; 297:291–5.
https://doi.org/10.1016/0003-9861(92)90675-M


112. Tizkar B, Kazemi R, Alipour A, Seidavi A, Naseralavi G, Ponce-Palafox JT. Effects of dietary supplementation with astaxanthin and β-carotene on the semen quality of goldfish (carassius auratus). Theriogenology 2015; 84:1111–7.
https://doi.org/10.1016/j.theriogenology.2015.06.011


113. Comhaire F, Garem YE, Mahmoud A, Eertmans F, Schoonjans F. Combined conventional/antioxidant “astaxanthin” treatment for male infertility: A double blind, randomized trial. Asian J Androl 2005; 7:257–62.
https://doi.org/10.1111/j.1745-7262.2005.00047.x


114. Vahidinia A, Rahbar AR, Shakoori Mahmoodabadi MM. Effect of astaxanthin, vitamin E, and vitamin C in combination with calorie restriction on sperm quality and quantity in male rats. J Diet Suppl 2017; 14:252–63.
https://doi.org/10.1080/19390211.2016.1211783


115. Bahmanzadeh M, Vahidinia A, Mehdinejadiani S, Shokri S, Alizadeh Z. Dietary supplementation with astaxanthin may ameliorate sperm parameters and DNA integrity in streptozotocin-induced diabetic rats. Clin Exp Reprod Med 2016; 43:90–6.
https://doi.org/10.5653/cerm.2016.43.2.90



116. Fang Y, Zhong R, Chen L, Feng C, Sun H, Zhou D. Effects of astaxanthin supplementation on the sperm quality and antioxidant capacity of ram semen during liquid storage. Small Rumin Res 2015; 130:178–82.
https://doi.org/10.1016/j.smallrumres.2015.05.016

117. Guo HT, Wang JT, Sun LZ, et al. Effects of astaxanthin on plasma membrane function and fertility of boar sperm during cryopreservation. Theriogenology 2021; 164:58–64.
https://doi.org/10.1016/j.theriogenology.2021.01.007


118. Qamar AY, Fang X, Bang S, Shin ST, Cho J. The effect of astaxanthin supplementation on the post-thaw quality of dog semen. Reprod Domest Anim 2020; 55:1163–71.
https://doi.org/10.1111/rda.13758


119. Abdi-Benemar H, Khalili B, Zamiri MJ, et al. Effects of astaxanthin supplementation on the freezability, lipid peroxidation, antioxidant enzyme activities and post-thawing fertility of ram semen. Small Rumin Res 2020; 192:106213
https://doi.org/10.1016/j.smallrumres.2020.106213

120. Eser A, Aydemir T. The effect of kinetin on wheat seedlings exposed to boron. Plant Physiol Biochem 2016; 108:158–64.
https://doi.org/10.1016/j.plaphy.2016.06.024


121. Olsen A, Siboska GE, Clark BFC, Rattan SIS. N6-furfuryladenine, kinetin, protects against fenton reaction-mediated oxidative damage to DNA. Biochem Biophys Res Commun 1999; 265:499–502.
https://doi.org/10.1006/bbrc.1999.1669


122. Abdel-Latif R, Fathy M, Anwar HA, Naseem M, Dandekar T, Othman EM. Cisplatin-induced reproductive toxicity and oxidative stress: Ameliorative effect of kinetin. Antioxidants 2022; 11:863
https://doi.org/10.3390/antiox11050863



123. Qamar AY, Fang X, Bang S, Kim MJ, Cho J. Effects of kinetin supplementation on the post-thaw motility, viability, and structural integrity of dog sperm. Cryobiology 2020; 95:90–6.
https://doi.org/10.1016/j.cryobiol.2020.05.015


124. Zadeh Hashem E, Eslami M. Kinetin improves motility, viability and antioxidative parameters of ram semen during storage at refrigerator temperature. Cell Tissue Bank 2018; 19:97–111.
https://doi.org/10.1007/s10561-016-9604-3


125. Bevilacqua A, Carlomagno G, Gerli S, et al. Results from the international consensus conference on myo-inositol and d-chiro-inositol in obstetrics and gynecology–assisted reproduction technology. Gynaecol Endocrinol 2015; 31:441–6.
https://doi.org/10.3109/09513590.2015.1006616

126. Artini PG, Casarosa E, Carletti E, Monteleone P, Noia AD, Berardino OMD. In vitro effect of myo-inositol on sperm motility in normal and oligoasthenospermia patients undergoing in vitro fertilization. Gynaecol Endocrinol 2017; 33:109–12.
https://doi.org/10.1080/09513590.2016.1254179

127. Calogero AE, Gullo G, La Vignera S, Condorelli RA, Vaiarelli A. Myoinositol improves sperm parameters and serum reproductive hormones in patients with idiopathic infertility: a prospective double-blind randomized placebo-controlled study. Andrology 2015; 3:491–5.
https://doi.org/10.1111/andr.12025


128. Condorelli RA, La Vignera S, Di Bari F, Unfer V, Calogero AE. Effects of myoinositol on sperm mitochondrial function in-vitro. Eur Rev Med Pharmacol Sci 2011; 15:129–34.

129. Condorelli RA, La Vignera S, Bellanca S, Vicari E, Calogero AE. Myoinositol: Does it improve sperm mitochondrial function and sperm motility? Urology 2012; 79:1290–5.
https://doi.org/10.1016/j.urology.2012.03.005


130. Qamar AY, Fang X, Kim MJ, Cho J. Myoinositol supplementation of freezing medium improves the quality-related parameters of dog sperm. Animals 2019; 9:1038
https://doi.org/10.3390/ani9121038



131. Doğu Z, Şahinöz E, Aral F, Koyuncu İ, Yüksekdağ Ö. Effects of inositol supplementation in sperm extender on the quality of cryopreserved mesopotamian catfish (silurus triostegus, h. 1843) sperm. Animals 2021; 11:3029
https://doi.org/10.3390/ani11113029



132. Vash NT, Nadri P, Karimi A. Synergistic effects of myo-inositol and melatonin on cryopreservation of goat spermatozoa. Reprod Domest Anim 2022; 57:876–85.
https://doi.org/10.1111/rda.14131


133. Abdolsamadi M, Mohammadi F, Nashtaei MS, et al. Does myoinositol supplement improve sperm parameters and DNA integrity in patients with oligoasthenoteratozoospermia after the freezing–thawing process? Cell Tissue Ban 2020; 21:99–106.
https://doi.org/10.1007/s10561-019-09801-7

134. Ponchia R, Bruno A, Renzi A, et al. Oxidative stress measurement in frozen/thawed human sperm: The protective role of an in vitro treatment with myo-inositol. Antioxidants 2022; 11:10
https://doi.org/10.3390/antiox11010010



135. Johinke D, De Graaf SP, Bathgate R. Quercetin reduces the in vitro production of H2O2 during chilled storage of rabbit spermatozoa. Anim Reprod Sci 2014; 151:208–19.
https://doi.org/10.1016/j.anireprosci.2014.10.017


136. Seifi-Jamadi A, Ahmad E, Ansari M, Kohram H. Antioxidant effect of quercetin in an extender containing dma or glycerol on freezing capacity of goat semen. Cryobiology 2017; 75:15–20.
https://doi.org/10.1016/j.cryobiol.2017.03.002


137. Avdatek F, Yeni D, İnanç ME, et al. Supplementation of quercetin for advanced DNA integrity in bull semen cryopreservation. Andrologia 2018; 50:e12975
https://doi.org/10.1111/and.12975

138. Bang S, Qamar AY, Tanga BM, et al. Quercetin improves the apoptotic index and oxidative stress in post-thaw dog sperm. Environ Sci Pollut Res 2022; 29:21925–34.
https://doi.org/10.1007/s11356-021-17421-6

139. Zribi N, Chakroun NF, Abdallah FB, et al. Effect of freezing–thawing process and quercetin on human sperm survival and DNA integrity. Cryobiology 2012; 65:326–31.
https://doi.org/10.1016/j.cryobiol.2012.09.003


140. Gibb Z, Butler TJ, Morris LHA, et al. Quercetin improves the postthaw characteristics of cryopreserved sex-sorted and nonsorted stallion sperm. Theriogenology 2013; 79:1001–9.
https://doi.org/10.1016/j.theriogenology.2012.06.032


141. Qazi IH, Angel C, Yang H, et al. Role of selenium and selenoproteins in male reproductive function: a review of past and present evidences. Antioxidants 2019; 8:268
https://doi.org/10.3390/antiox8080268



142. Noack-Füller G, De Beer C, Seibert H. Cadmium, lead, selenium, and zinc in semen of occupationally unexposed men. Andrologia 1993; 25:7–12.
https://doi.org/10.1111/j.1439-0272.1993.tb02674.x


143. Ghafarizadeh AA, Vaezi G, Shariatzadeh MA, Malekirad AA. Effect of in vitro selenium supplementation on sperm quality in asthenoteratozoospermic men. Andrologia 2018; 50:e12869
https://doi.org/10.1111/and.12869

144. Powell SR. The antioxidant properties of zinc. J Nutr 2000; 130:1447S–54S.
https://doi.org/10.1093/jn/130.5.1447S


145. Wu J, Wu S, Xie Y, et al. Zinc protects sperm from being damaged by reactive oxygen species in assisted reproduction techniques. Reprod Biomed Online 2015; 30:334–9.
https://doi.org/10.1016/j.rbmo.2014.12.008


146. Chia SE, Ong CN, Chua LH, Ho LM, Tay SK. Comparison of zinc concentrations in blood and seminal plasma and the various sperm parameters between fertile and infertile men. J Androl 2000; 21:53–7.
https://doi.org/10.1002/j.1939-4640.2000.tb03275.x


147. Omu A, Al-Azemi M, Kehinde EO, Anim JT, Oriowo MA, Mathew TC. Indications of the mechanisms involved in improved sperm parameters by zinc therapy. Med Princ Pract 2008; 17:108–16.
https://doi.org/10.1159/000112963


148. Talevi R, Barbato V, Fiorentino I, Braun S, Longobardi S, Gualtieri R. Protective effects of in vitro treatment with zinc, d-aspartate and coenzyme q10 on human sperm motility, lipid peroxidation and DNA fragmentation. Reprod Biol Endocrinol 2013; 11:81
https://doi.org/10.1186/1477-7827-11-81



149. Berkovitz A, Allouche-Fitoussi D, Izhakov D, Breitbart H. Cryopreservation of human sperm in the presence of zn2+ increases the motility rate. J Obstet Gynecol Invest 2018; 1:e6–12.
https://doi.org/10.5114/jogi.2018.73423

150. Reddy VS, Yadav B, Yadav CL, et al. Effect of sericin supplementation on heat shock protein 70 (hsp70) expression, redox status and post thaw semen quality in goat. Cryobiology 2018; 84:33–9.
https://doi.org/10.1016/j.cryobiol.2018.08.005


151. Kumar P, Kumar D, Sikka P, Singh P. Sericin supplementation improves semen freezability of buffalo bulls by minimizing oxidative stress during cryopreservation. Anim Reprod Sci 2015; 152:26–31.
https://doi.org/10.1016/j.anireprosci.2014.11.015


152. Raza S, Uçan U, Aksoy M, Erdoğan G, Ceylan A, Serin I. Silk protein sericin pretreatment enhances osmotic tolerance and post-thaw sperm quality but reduces the ability of sperm cells to undergo in vitro induced acrosome reaction in rabbit. Cryobiology 2019; 90:1–7.
https://doi.10.1016/j.cryobiol.2019.09.008


153. Nasirabadi MH, Shirazi A, Kadivar A, et al. Sericin ameliorates the capacitation state and chromatin integrity of frozen-thawed stallion spermatozoa by reducing oxidative stress. Avicenna J Med Biotechnol 2019; 11:245–52.


154. Foote RH, Brockett CC, Kaproth MT. Motility and fertility of bull sperm in whole milk extender containing antioxidants. Anim Reprod Sci 2002; 71:13–23.
https://doi.org/10.1016/S0378-4320(02)00018-0


155. Shabanian S, Farahbod F, Rafieian M, Ganji F, Adib A. The effects of vitamin c on sperm quality parameters in laboratory rats following long-term exposure to cyclophosphamide. J Adv Pharm Technol Res 2017; 8:73–9.
https://doi.org/10.4103/japtr.JAPTR_153_16



156. Scott R, MacPherson A, Yates R, et al. The effect of oral selenium supplementation on human sperm motility. Br J Urol 1998; 82:76–80.
https://doi.org/10.1046/j.1464-410x.1998.00683.x


157. Lewin A, Lavon H. The effect of coenzyme q10 on sperm motility and function. Mol Aspects Med 1997; 18:213–9.
https://doi.org/10.1016/S0098-2997(97)00036-8

158. Donà G, Kožuh I, Brunati AM, et al. Effect of astaxanthin on human sperm capacitation. Mar Drugs 2013; 11:1909–19.
https://doi.org/10.3390/md11061909



- TOOLS
-
METRICS

- Related articles
-
Role of oxytocin in improving the welfare of farm animals — A review2017 April;30(4)






 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print




